| Author | Ruru Ping1, Takashi Oshio2 1Graduate School of Economics, Hitotsubashi University, Tokyo, Japan 2Institute of Economic Research, Hitotsubashi University, Tokyo, Japan |
|---|---|
| Overview | The long-term care (LTC) system in Japan, which was introduced in 2000, is characterised by a national compulsory long-term care insurance (LTCI) system, administrated by municipalities under the guidance of the central government. The system is financed through a mixed system, which includes taxation, LTCI, and user coinsurance. It covers those aged 65 and older, and people aged 40 to 64 with certain ageing-related diseases. A comprehensive needs assessment is required for in-kind benefits. Japan’s formal LTC relies heavily on home- and community-based care. The residential care market is subject to strict regulations for for-profit companies to enter the market. Since 2015, the Japanese government has been committed to establishing a community-based integrated care system in response to the rising burden of non-communicable diseases and to promote healthy ageing in place. In recent years, there has been a growing emphasis on preventive care aimed at preventing frailty and delaying the onset of dependency. In 2019, long-term care spending in Japan accounted for 2% of the total Gross Domestic Product (GDP) in 2019, which is above the OECD average[1] |
| Governance and system organisation | According to the Long-Term Care Insurance Act, passed in 1997 and effective from 2000, municipal governments serve as insurers of long-term care insurance (LTCI); the national government is responsible for implementing measures to ensure the provision of health services, public aid services, and all other necessary actions for the smooth and efficient operation of LTC plans; prefectural governments are tasked with providing necessary advice and appropriate support to facilitate the operation of LTC plans[2]. LTCI is a nationally regulated system, but its administration is decentralised[3]. Specifically, municipal governments formulate an LTC service plan that is updated every three years. They are responsible for setting up a specific account for LTCI, determining insurance premiums by considering the types of services provided to older residents and their needs, and collecting the premiums. Municipal and prefectural governments are required to update their LTC service plans and submit them to the Ministry of Health, Labour and Welfare (MHLW) every three years. The Health and Welfare Bureau for the Elderly within the MHLW serves as the key central government agency responsible for various aspects of the LTC system. Its responsibilities include determining the menu of available LTC services and their prices on a nationwide scale, regulating the eligibility criteria for service providers, and setting standards for LTC services. Additionally, the MHLW regulates the adoption of innovative technology in LTC settings, such as care robots, and implements policies for the integration of health care and LTC[4] |
| Financing and coverage | LTC in Japan is financed through a mixed system, which includes taxation, long-term care insurance (LTCI), and user coinsurance[5]. Half of the financing comes from taxes, with 25% contributed by the central government, 12.5% by prefectures, and another 12.5% by municipalities. The remaining half is funded through premium contributions from individuals aged 40 years old and above. Enrolees in LTCI are divided into two categories: (1) older people aged 65 years and above, whose premiums are withheld from their pension payments by municipalities, and (2) individuals aged 40-64 years old with ageing-related diseases, who are concurrently enrolled in medical insurance schemes, and the health insurers levy the premium by adding it to the health insurance premium. The premium rate for category 2 (40-64 years old) varies based on the type of employment. For large companies (Kumiai Kempo), the premium rate differs among insurers and falls within the range of 1.6-2.0% (shared equally between the employer and employee) for approximately 90% of firms in 2022. The premium rate for small and medium-sized enterprises (Kyokai Kempo) is uniform at 1.82% (shared equally between the employer and employee) in 2022. The premiums of self-employed individuals depend on their income and other factors, varying by municipality. For those in category 1 (65+), the premium is linked to income and varies by municipality. The average premium amounts to 6,014 JPY per month, with a wide range of 2,200-9,800 JPY in 2022. Those who want to receive in-kind benefits (i.e., care services) are required to apply to the municipal government and undergo a comprehensive needs assessment. Users are responsible for a range of 10% to 30% coinsurance for LTC services depending on their income level[6], and they are also responsible for covering the costs of residence and food in institutional settings[5]. Co-payments are capped at fixed monthly level on a sliding scale based on income level[3]. |
| Service Delivery | |
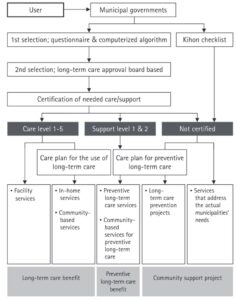
| Service Delivery Overview | LTC services in Japan encompass a range of options, including in-home services, community-based services, and facility services[7]. It should be noted that these services are provided only in kind; cash benefits are not allowed. As shown in Figure 1, these services are available to insured individuals who have been certified for care or support needs. Japan’s long-term care insurance (LTCI) system classified LTC needs into seven levels, which require certification: support levels 1 and 2, as well as care needs levels 1 (least dependent) to 5 (most dependent). Service users have the freedom to select any LTC provider and choose the type and frequency of services within benefit limits determined by their eligibility status, which is determined through a needs assessment[8]. Individuals who do not qualify for LTC or support may use preventive services within the community. Overall, Japan’s formal LTC relies heavily on home- and community-based care, which implies that family members provide informal care at least to some extent to complement formal care. In recent years, there has been a growing emphasis on preventive care aimed at delaying the onset of dependency. Figure 1. Procedure for use of LTC services in Japan
|
| Community-based care | In-home services include home-visit services (e.g., housekeeping, home-visit bathing, and home-visit nursing care), day care (e.g., outpatient day care, outpatient rehabilitation, outpatient preventive services), and short-stay services (e.g., short-term admission for daily life LTC). Community-based services include multi-functional care services in small group homes, home-visit care at night, communal daily care for people living with dementia, and some preventive services[5]. The largest portion of LTC services is provided through home- and community-based care in Japan. According to MHLW’s statistics, out of 4.59 million LTC recipients, 3.34 million were receiving home-based care, 0.90 million were receiving community-based care, and 0.96 million were receiving facility-based care, as of March 2023[9]. The introduction of LTCI in 2000 encouraged new providers, including for-profit ones, to enter the home- and community-based care market and compete with traditional public social welfare providers[8]. As a result, numerous for-profit providers have entered this market following the introduction of LTCI, and the volume of services has also expanded substantially[10]. The number of home-care visits increased from 1,240,000 in 2000 to 3,890,000 in 2015[8]. However, during the COVID-19 pandemic, a significant reduction in the use of outpatient and short-stay services has been observed in 2020, although longer-term impacts need to be further investigated[11]. The increase in frailty among older people is also concerning due to COVID-19 pandemic. With regard to this, the group activities called “Kayoi-no-ba” at healthcare facility in local community through physical exercise, hobbies, or other activities may play a prominent role in preventing the onset and progression of frailty among community-dwelling older adults[12]. |
| Residential care settings | Institutional care settings in Japan are classified into three types of nursing homes, which include LTC welfare facilities for older people (aka. special nursing homes), LTC health facility for older people (aka., geriatric health service facilities), and LTC medical facilities (i.e., medical LTC sanatoriums)[13],[5],[7]. Most older residents admitted to LTC welfare facilities reside there for the remainder of their lifetime. LTC health facilities are designed for rehabilitation to smoothly transition from the hospital to the home. In LTC medical facilities, medical care is offered under the national health care system rather than the LTC system. Given strict regulations for for-profit companies to enter the care market for individuals with high nursing and medical needs, most nursing homes in Japan are non-profit social welfare or medical institutions. For-profit facilities need to obtain a license issued by their prefectural government, and even with a license, they have to contract with other licensed LTC providers if their residents need nursing care. Residential care providers are paid based on a national fee schedule.[3] |
| Assistive technology | In Japan, individuals with disabilities (PWD) in need of assistive products can either lease the products from the municipal governments or purchase them from designated providers. The general payment arrangement is that the user contributes 10% of the costs, while public services cover the remaining 90%[14]. The funding for these services is shared among the central, prefectural and municipal governments in the ratio of 2:1:1. The provision of assistive products is primarily governed under the Long-term Care Insurance Act and Services and Supports for PWDs Act. |
| Workforce | In 2019, Japan had seven formal LTC workers per 100 people aged 65 and over[15]. Like many other countries, Japan is facing a shortage of formal care workers and high turnover rate. It is estimated that by 2023, there will be a shortage of 220,000 workers, which is expected to increase to 320,000 by 2025 and reach 690,000 by 2040[16]. The turnover rate among care workers was approximately 15% during 2012–2016[17]. Several factors contribute to the high turnover rate, including low income, illness or old age, responsibilities such as caring for an aged or sick family member, childcare, the short tenure of contract, and workplace interpersonal problems [17], [18]. The majority of care workers in Japan are female. In 2021, only 12.5% of total home care workers and 23.8% of nursing care workers were male[19]. The average age of care workers in home-based settings was 54.4 years old and was 47.3 years old in nursing homes[20]. Notably, female care workers, who accounted for the majority of the care workforce, are ageing rapidly[18]. As for payment, in 2021, the average wage for home care workers was approximately $1,720 per month, and for nursing care workers, it was $1,710. These wages were lower than the average monthly salary in Japan, which was $2,365[17]. Moreover, the older a prefecture’s population, the higher the ratio of workers in the care industry; however, the overall wage rate tends to be lower, making the industry less attractive in the labour market, particularly for males[18]. In Japan, the ‘certified care worker’ is a distinct professional endorsed by the Social Welfare Worker and Certified Care Worker Act and has a unique career path from entry-level to expert-level, known as the ‘Long-term Care Professional Career Grade System’, although only the first four levels have been widely assessed so far[21]. The assessment consists of examinations of both knowledge and practical skills. It is possible to work in LTC facilities without qualification in Japan[17]. As of 2021, 0.6% and 14% of care workers are working without qualifications[19]. However, at least Level 1 certification is required to provide physical care that involves touching a person’s body[20]. Japan’s certified care worker qualification system provides several pathways for candidates to apply for the national examination to obtain the Level 4 certification[21]. To address the workforce shortage, the Japanese government has been opening up its labour market for foreign care workers, providing four pathways to become a qualified care worker in Japan[22]. These pathways include bilateral programmes based on the Economic Partnership Agreement with Indonesia (2008), the Philippines (2009), and Vietnam (2014). Additionally, the three other pathways have been in effect since 2017: the new resident status of ‘Care Worker’, the new occupation category under the Technical Intern Training Programme, the new resident status of ‘Specified Skilled Workers’. Each route has its application process, requirements, and period of stay. Nonetheless, the retention rate of these candidates was very low (only 40%), and qualified care workers often return to their home countries after their employment contracts end[17]. To mitigate the shortage of care workers, the government has been exploring the application of high technology in care settings to increase productivity. Accordingly, educational and training programmes for care workers need to incorporate components of care services using information and communication technology (ICT) and robotics[22]. In Japan, care managers play a crucial role in actively participating in care plans and service arrangements[7]. The qualification as a care manager can be obtained by medical professionals or care workers upon successfully completing the respective prefectural-level exam[23]. Care managers coordinate a wide range of services from different providers, taking into account the geographically dispersed home settings while staying within the allocated budget. They evaluate older adults in need of nursing care based on the written opinion from attending physician and develop a comprehensive plan that includes appropriate nursing care, rehabilitation, and other necessary services[20]. The care plan is tailored to the specific needs and intentions of older persons and their families. Nurses, physical therapists, occupational therapists, and certified care workers are responsible for delivering care and rehabilitation to the older person, following the care plan created by the care manager[20]. They work collaboratively to ensure the provision of high-quality, people-centred care to meet the needs of older adults. The extent to which Japan’s LTC system relies on unpaid care remains unclear[3]. The introduction of the LTCI system aimed to shift the burden of family caregiving to social solidarity by providing in-kind benefits[7]. In 1995, Japan enacted the Child Care and Family Care Leave Act, which went into effect in 1999, as a supportive policy for flexible work arrangements. This act allows employees with family members in need of care to take time off work to make the necessary arrangements, enabling them to balance employment and caregiving responsibilities in the future. Since then, the government has made several amendments to better meet the needs of affected families[24]. Under the existing system, employees can take up to three instalments of caregiver leave, totalling 93 days per family member in need of care[20]. Nonetheless, the 10% coinsurance requirement may deter the low-income subpopulation from seeking formal services and tend to heavily rely on unpaid family care[3]. This situation can be particularly pronounced for women, given the Japanese tradition where the wife of the oldest son is traditionally expected to be responsible for the daily care of her husband’s parents[25]. Ample evidence has shown the adverse effects of family caregiving on the wellbeing, social life, and labour participation of caregivers among Japanese population[26],[27],[28] . This may pose an equity challenge if no more effective measures are taken to support informal caregivers. |
| Information systems | In 2018, the Japanese government allocated funds for the project of constructing long-term care (LTC) databases, as they were previous underdeveloped compared to the medical sector[29]. This initiative was followed by the Revision of Long-term Care Insurance (LTCI) Law in 2018, which stipulates that prefectures and municipalities must implement the Plan-Do-Check-Action (PDCA) approach in managing their LTCI plans[20]. The LTCI databases include a LTCI comprehensive database, a VISIT (monitoring and evaluation for rehabilitation services for LTC), and CHASE (care, health status and events)[6]. These databases are designed to collect and analyse data on the conditions of older people and the content of LTC services, thereby facilitating evidence-based policymaking and practices[29]. In 2021, a major amendment to the LTCI was made to further develop data infrastructure for promoting the integration of health care and LTC systems[6]. |
| New models of care and innovations | Following the revision of Japan’s Long-term Care Insurance (LTCI) Law in 2015, the country’s LTC system introduced the Comprehensive Service for Preventive Care and Daily Life Support service model[29],[30]. This innovative model emphasizes community engagement and mobilisation to enable the delivery of diverse care services for older adults, provided not only by care professionals but also by local citizens. It promotes mutual aid in local communities, tailoring care services to local contexts, particularly considering regional disparities between urban and rural areas in Japan. These disparities are prominent in terms of public transportation network, population ageing rate, and community solidarity. Under this service model, municipal governments serve as organisers of service provision. For instance, services like ‘removing furniture’, which were not covered by existing in-home care services, may be provided by local residents with municipal subsidies. This model is considered cost-effective, as it encourages increased social participation of the active, healthy older individuals in community services, benefiting for their health and wellbeing while also promoting community solidarity[29]. In recognition of the pressing public health and social issues brought on by the rising burden of dementia, the Cabinet enacted the National Framework for Promoting Dementia Care in 2019, which is effective until 2025[31],[32]. The framework emphasizes prevention and inclusion, aiming to delay the onset of dementia and foster a society where people can live their daily lives with hope and dignity, even if they are living with dementia[20]. The Framework consists of five pillars: (1) promoting public awareness and supporting efforts to hear from people living with dementia; (2) prevention; (3) supporting healthcare, caregiving, and LTC services and providers; (4) promoting the creation of barrier-free spaces and services for people living with dementia, supporting those with early-onset dementia, and encouraging social participation; and (5) promoting research and development, industry advancements, and international dissemination of research results[33]. In 2020, the Japanese government promoted the introduction of information and communication technology (ICT), robots, AI, and other tools in nursing care settings to complement the work previously carried out by human staff. However, these tools are subject to strict regulations[34]. |
| Performance | |
| Affordability & equity | There are several concerns regarding the performance of LTC system in Japan. Firstly, according to the Ministry of Health, Labour and Welfare, the productivity of medical and LTC services in Japan was found to be lower than that in other major developed economies[35]. One reason for this low productivity is the excessive burden imposed by handwritten care records. Secondly, fiscal deterioration is worrisome. The government’s gross debt-to-GDP ratio reached 256.9 in 2021, standing at the highest level among major developed economies[36]. On the other hand, spurred by advanced population ageing, LTC expenditures have increased remarkably from USD$32.7 billion in 2000 when LTCI was introduced to USD$106.4 billion in 2019, with projections to further exceed USD$136.4 billion by 2025[7]. Correspondingly, premiums have increased, and the coinsurance rate has also increased for certain income level populations. Thirdly, significant regional disparities exist regarding LTC cost per beneficiary and certification rate per first insured person, with considerable variation across prefectures[29]. These regional variations may diminish the equity of the LTC system in Japan. |
| Effectiveness | Japan has a structure-process-outcome evaluation system for its long-term care insurance (LTCI) system[29]. The government revised its LTCI law in 2018, leading to the introduction of an outcome indicator for evaluating the performance of day-care services and the launch of two national evaluation systems using process indicators. However, the use of outcome measures is controversial due to concerns about unintended consequences, such as cream skimming. Regarding the national process evaluation systems, one evaluates the efforts of municipalities and prefectures to support self-reliance and prevent the deterioration of the LTCI system, offering financial incentives called the Insurer Function Promotion Grants based on performance. The other system, known as business evaluation, aims to strengthen regional Comprehensive Support Centres nationwide. Municipalities must take necessary measures, such as revising their management policies annually, based on the self-evaluation of Community Support Centres, to improve their operations.
|
| New reforms and policies | To contain costs, the government has increased the coinsurance rate from 10% for all individuals to 20% for those with incomes above a certain level since 2015, and further raised to 30% for those with the highest income and/or asset levels after 2018[37]. In 2015, Japan revised its Medical Care Act and LTCI Law to establish a Community-based Integrated Care System by 2025, in response to the rising burden of non-communicable diseases and to promote healthy ageing in place[29],[7]. This system involves the integration of medical care, LTC, preventive care, livelihood support, and housing services. Prefectures are responsible for establishing the Community-based Integrated Care System based on regional autonomy and independence[5]. Japan has revised its LTC remuneration in recent years (2014-2015, 2017-2019, 2021). The latest revision was in 2021 following the onset of COVID-19 pandemic. The government considered the situation regarding the management of care providers, including the impact of price trends on property costs, while also taking into account the need to recruit and improve the treatment of care staff, resulting in a 0.7% increase in LTC renumeration[6]. In addition, the government has been discussing the employment of a task shifting approach to alleviate the strain on human resources, particularly the high skilled medical specialists[38] |
| Suggested Citation | Ping, R. and Oshio T. (2023) Long-Term Care System Profile: Japan. Global Observatory of Long-Term Care, Care Policy & Evaluation Centre, London School of Economics and Political Science. https://goltc.org/system-profile/japan/ |
| Key Sources | Estevez-Abe M., Ide H., Curry N., Hemmings N. and Comas-Herrera A. (2021). COVID-19 and the Long-Term Care system in Japan. In: Comas-Herrera A., Marczak J., Byrd W., Lorenz-Dant K., Pharoah D. (editors) LTCcovid International Living report on COVID-19 and Long-Term Care. LTCcovid, Care Policy and Evaluation Centre, London School of Economics and Political Science. https://ltccovid.org/covid-19-and-the-long-term-care-system-in-japan/ Masui, H., Otaga, M., Moriyama, Y., & Matsushige, T. (2019). Current issues in long-term care policy and research: Toward the promotion of evidence-based policy. 保健医療科学,1: 34-44. https://www.niph.go.jp/journal/data/68-1/201968010006.pdf Ministry of Health, Labour and Welfare, Japan. (2016). Long-term care insurance system of Japan. Available at: https://www.mhlw.go.jp/english/policy/care-welfare/care-welfare-elderly/dl/ltcisj_e.pdf (accessed 14 July 2023). Yamada, M., & Arai, H. (2020). Long-Term Care System in Japan. Annals of Geriatric Medicine and Research, 24(3), 174–180. https://doi.org/10.4235/agmr.20.0037 |
| References | [1] OECD. (2021). Health at a glance 2021: Highlights for Japan. Available at: https://www.oecd.org/japan/health-at-a-glance-Japan-EN.pdf (accessed 14 July, 2023). [2] Ministry of Justice, Japan (MoJ). (1997). Long-Term Care Insurance Act. Available at: https://www.ilo.org/dyn/natlex/docs/ELECTRONIC/50024/96299/F108480626/JPN50024.pdf (accessed 14 July 2023). [3] Estevez-Abe M., Ide H., Curry N., Hemmings N. and Comas-Herrera A. (2021). COVID-19 and the Long-Term Care system in Japan. In: Comas-Herrera A., Marczak J., Byrd W., Lorenz-Dant K., Pharoah D. (editors) LTCcovid International Living report on COVID-19 and Long-Term Care. LTCcovid, Care Policy and Evaluation Centre, London School of Economics and Political Science. https://ltccovid.org/covid-19-and-the-long-term-care-system-in-japan/ [4] Ministry of Health, Labour and Welfare, Japan (MHLW). (2022). Service Guide 2022. Available at: https://www.mhlw.go.jp/english/org/pamphlet/dl/serviceguide2022.pdf (accessed 14 July 2023). [5] Ministry of Health, Labour and Welfare, Japan (MHLW). (2016). Long-term care insurance system of Japan. Available at: https://www.mhlw.go.jp/english/policy/care-welfare/care-welfare-elderly/dl/ltcisj_e.pdf (accessed 14 July 2023). [6] Ministry of Health, Labour and Welfare, Japan (MHLW). (2022). Recent developments in the long-term care insurance system介護保険制度をめぐる最近の動向について. Available at: https://www.mhlw.go.jp/content/12300000/000917423.pdf (accessed 14 July 2023). [7] Yamada, M., & Arai, H. (2020). Long-term care system in Japan. Annals of Geriatric Medicine and Research, 24(3), 174–180. https://doi.org/10.4235/agmr.20.0037 [8] Shibuya, K., Gilmour, S., & Tatara, K. (eds.) (2018). Japan Health System Review. World Health Organisation, Regional Office for South–East Asia. ISBN 978–92-9022–626-0. Available at: https://www.ecoi.net/en/file/local/2018218/B5390.pdf [9] Ministry of Health, Labour and Welfare, Japan. (2023). Summary of the results of the Monthly Report of Actual Statistics on Nursing Care Benefit Expenses (March 2023 review) 介護給付費等実態統計月報(令和5年3月審査分)結果の概要. Available at: https://www.mhlw.go.jp/toukei/saikin/hw/kaigo/kyufu/2023/dl/202303_gaiyou.pdf (accessed 23 July 2023). [10] Kubo, M. (2014). Long-term care insurance and market for aged care in Japan: Focusing on the status of care service providers by locality and organisational nature based on survey results. Australasian Journal on Ageing, 33(3), 153–157. https://doi.org/10.1111/ajag.12038 [11] Sato, K., Niimi, Y., Iwatsubo, T., & Ishii, S. (2022). Change in long‐term care service usage in Japan following the COVID‐19 pandemic: A survey using a nationwide statistical summary in 2018–2021. Geriatrics & Gerontology International, 22(9), 803-809. https://doi.org/10.1111/ggi.14461 [12] Kojima, M., Satake, S., Osawa, A., & Arai, H. (2021). Management of frailty under COVID-19 pandemic in Japan. Global Health & Medicine, 3(4), 196-202. https://www.jstage.jst.go.jp/article/ghm/3/4/3_2020.01118/_article [13] Shimizutani, S. (2014). The future of long-term care in Japan, Asia–Pacific Review, 21: 88-119, DOI: 10.1080/13439006.2014.925199 [14] WHO Collaborating Centres In The Western Pacific Region. (2013). Sharing Good Practice In Rehab Between The Western Pacific WHO CCs: E-Newsletter- Issue No. 4 (June, 2013). Available at: http://www.rehab.go.jp/english/whoclbc/doc/JoiningHands4.pdf (accessed 14 July, 2023). [15] OECD (2021). OECD Health Statistics. Available at: https://www.oecd.org/health/health-systems/long-term-care-workforce.htm (accessed 14 July 2023). [16] Ministry of Health, Labour and Welfare (MHLW). (2021). The number of caregivers required according to the 8th Long-Term Care Insurance Business Plan 第8期介護保険事業計画に基づく介護職員の必要数について [17] Takeda, S. (2023). Factors related to turnover and intention to leave the care working profession in Japan: A Review. Yonago Acta Medica, 66(2), 196–201. https://doi.org/10.33160/yam.2023.05.001 [18] Yamada, A. and Ishii, K. (2021). Aging and wages of long-term care workers: A case study of Japan, 2002–2017. Economic Analysis, Economic and Social Research Institute, Cabinet Office内閣府経済社会総合研究所『経済分析』,202. Available at: https://www.esri.cao.go.jp/jp/esri/archive/bun/bun202/bun202d.pdf [19] Care Work Foundation. (2021) Report of Care Labour Survey in Care Facilities 事業所における介護労働実態調査結果報告書. Tokyo: Care Work Foundation. Available from: http://www.kaigo-center.or.jp/report/pdf/2022r01_chousa_jigyousho_kekka.pdf [20] Ibid [21] Elderly Service Providers Association (ESPA; シルバーサービス振興会). (2023). Long-term Care Professional Career Grade System (介護プロフェッショナルキャリア段位制度). Tokyo: Elderly Service Providers Association. Available at: https://careprofessional.org/careproweb/summary (accessed 14 July 2023). [22] Ogawa, T. and Komazawa, O. (2021). Qualifications Framework for Long-term Care Workers in India, Japan, and the Philippines. Economic Research Institute for ASEAN and East Asia (ERIA): Indonesia. Available at: https://www.eria.org/uploads/media/Research-Project-Report/2021-09-Framework-Qualification-Long-term-Care-India-Japan-Philippines/Qualifications-Framework-for-Long-term-Care-Workers-India-Japan-Philippines.pdf (accessed 14 July 2023). [23] Shiota, S., Kitagawa, T., Hidaka, T., Goto, N., Mio, N., Kanai, K., Naka, M., Togino, H., Mochizuki, M., Ochikubo, H., Nakano, Y., Kihara, Y., & Kimura, H. (2021). The International Classification of Functioning, Disabilities, and Health categories rated as necessary for care planning for older patients with heart failure: A survey of care managers in Japan. BMC Geriatrics, 21(1), 704. https://doi.org/10.1186/s12877-021-02647-3 [24] Niimi, Y. (2021). Juggling paid work and elderly care provision in Japan: Does a flexible work environment help family caregivers cope? Journal of the Japanese and International Economies, 62, 101171. https://doi.org/10.1016/j.jjie.2021.101171 [25] Tsutsui, T., Muramatsu, N., & Higashino, S. (2014). Changes in perceived filial obligation norms among coresident family caregivers in Japan. The Gerontologist, 54(5), 797-807. https://doi.org/10.1093/geront/gnt093 [26] Oshio, T., & Kan, M. (2016). How do social activities mitigate informal caregivers’ psychological distress? Evidence from a nine-year panel survey in Japan. Health and quality of life outcomes, 14(1), 1-10. https://doi.org/10.1186/s12955-016-0521-8 [27] Oshio, T. (2015). How is an informal caregiver’s psychological distress associated with prolonged caregiving? Evidence from a six-wave panel survey in Japan. Quality of Life Research, 24, 2907-2915. https://doi.org/10.1007/s11136-015-1041-4 [28] Oshio, T., & Usui, E. (2018). How does informal caregiving affect daughters’ employment and mental health in Japan?. Journal of the Japanese and International Economies, 49, 1-7. https://doi.org/10.1016/j.jjie.2018.01.001 [29] Masui, H., Otaga, M., Moriyama, Y., & Matsushige, T. (2019). Current issues in long-term care policy and research: Toward the promotion of evidence-based policy. 保健医療科学,1: 34-44. https://www.niph.go.jp/journal/data/68-1/201968010006.pdf [30] Ministry of Health, Labour and Welfare, Japan (MHLW). (2018). Guidelines for comprehensive projects for care prevention and daily life support介護予防・日常生活支援総合事業のガイドラインについて. Available at: https://www.mhlw.go.jp/file/06-Seisakujouhou-12300000-Roukenkyoku/0000205730.pdf (accessed 14 July 2023). [31] Toba, K. (2021). Japan’s new framework on dementia care. Innovation in Aging, 5(Suppl 1), 383. https://doi.org/10.1093/geroni/igab046.1487 [32] Ministry of Health, Labour and Welfare, Japan (MHLW). (2019). Outline of Framework for Promoting Dementia Care認知症施策推進大綱. Available at: https://www.mhlw.go.jp/content/000522832.pdf (accessed 14 July 2023). [33] Kurita, S. (2023). The National Framework for Promotion of Dementia Policies. Available at: https://japanhpn.org/en/dementia1-3-2/ (accessed 14 July 2023). [34] Cabinet Office of Japan. (2020). Report on Promotion of Regulatory Reform. Available at: https://www8.cao.go.jp/kisei-kaikaku/english/pdf/200702/toshin.pdf (accessed 14 July 2023). [35] https://job.minnanokaigo.com/news/kaigogaku/no657/ [36] Ministry of Finance, Japan (MoF). (2022). The Japanese Public Finance Fact Sheet 2022. Available at: https://www.mof.go.jp/english/policy/budget/budget/fy2022/03.pdf (accessed 14 July 2023). [37] Ikegami, N. (2019). Financing Long-term Care: Lessons From Japan. International Journal of Health Policy and Management, 8(8), 462–466. https://doi.org/10.15171/ijhpm.2019.35 [38] Ministry of Health, Labour and Welfare, Japan (MHLW). (2018). Looking ahead to 2040, towards a society where everyone can be active and healthy for longer 2040年を展望し、誰もがより長く元気に活躍できる社会の実現に向けてAvailable at: https://www5.cao.go.jp/keizai-shimon/kaigi/minutes/2019r/0531/shiryo_02.pdf (accessed 14 July 2023). |
KEYWORDS / CATEGORIES | |
| Countries | Japan |